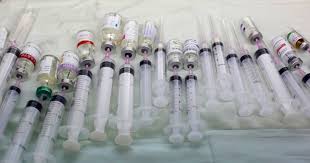
Unsafe Injections in Pakistan: Why Children Remain at Deadly Risk
One of Pakistan’s worst pediatric HIV epidemics struck Ratodero in 2019. Hundreds of kids tested positive for HIV, even though they had no conventional risk factors for transmission. Later studies revealed that the epidemic was largely caused by hazardous healthcare practices, notably the reuse of unsafe injection syringes and inadequate infection prevention and control (IPC) systems. Healthcare providers, lawmakers, and communities around the nation were horrified by the event.
In Taunsa, seven years later, similar fears reappeared of using unsafe injection. In healthcare institutions connected to a recent pediatric HIV epidemic, BBC News recently uncovered alarming data about syringe reuse, subpar sterilization procedures, and insufficient infection management measures. Between 2024 and 2025, over 300 children were said to have been diagnosed with HIV, which brought up challenging but crucial issues: Why are these preventable outbreaks still occurring? And what lessons are still to be learned?
A public health emergency that should not happen again

Major flaws in Pakistan’s healthcare system were brought to light by the HIV epidemic in Ratodero. In order to determine the underlying causes of transmission, the World Health Organization and national public health officials conducted research that revealed hazardous, unsafe injections and inadequate IPC adherence. Unregulated and informal healthcare practitioners continued to perform dangerous behaviors without accountability, and several medical facilities did not have adequate sterilization protocols.
The tragedy brought attention to a broader problem that is deeply ingrained in healthcare culture: the excessive use of injections. In many communities, injections are still seen as a “stronger” or quicker therapy than oral medicine. Even when they are not necessary, this notion promotes the use of injectable treatments. Repeated syringe usage and inadequate disposal practices, however, can transform regular healthcare into a source of infection rather than healing in resource-constrained environments.
The repeated incidence of unsafe injection-comparable epidemics following Ratodero indicates that long-term change has been restricted, even with increased global focus and public knowledge.
Unsafe Injection Practices: A Preventable Risk
Unsafe injection practices are not simply technological errors; they indicate flaws in healthcare systems, legislation, education, and accountability. The World Health Organization claims that dangerous injections contribute to the spread of bloodborne infections like HIV, hepatitis B, and hepatitis C.
Common hazardous practices include:
• Reusing needles or syringes between patients
• Inadequate medical equipment sterilization
• Hazardous disposal of waste from sharps
• A dearth of aseptic procedures and hand hygiene
• Insufficient personnel training on infection prevention
When appropriate IPC procedures are consistently applied, these behaviors are completely avoidable. Nevertheless, shortages of supplies, inadequate training, subpar monitoring systems, and a lack of enforcement at the primary healthcare level frequently cause gaps to persist.
The Importance of Nursing in Preventing Infections
The front lines of patient safety and infection control are still held by nurses. Their responsibilities include quality improvement, monitoring, advocacy, and education in addition to bedside treatment.
By making sure of the following, strong nursing practices can greatly lower healthcare-related infections:
Practices for Safe Injection
Nurses must adhere to single-use syringe policies and safe medication administration standards at all times. Treat every injection as a possible risk of infection if the necessary safeguards are disregarded.
Adherence to Hand Hygiene
The most effective approach to prevent healthcare-associated infections is still good hand hygiene. It is imperative to follow hand hygiene procedures religiously before and after interacting with patients.
Patient and Community Education
In addition, nurses are essential in educating patients and their families about the significance of getting treatment from knowledgeable medical professionals and about needless injections.
Support for More Robust IPC Systems
Healthcare professionals, particularly infection prevention nurses, have the power to promote improved training initiatives, supply availability, and institutional responsibility in regards to IPC compliance.
Frequently, infection prevention initiatives are unable to be put into practice in a sustainable manner due to a lack of empowered nursing leadership.
The Reasons Why Technology by Itself Is Insufficient
Healthcare systems today have access to superior surveillance systems, electronic reporting systems, and global IPC standards. Evidence-based guidance for safe healthcare delivery continues to be offered by organizations like the World Health Organization.
But guidelines alone cannot stop outbreaks unless they are consistently enforced and monitored. Even with written policies, adherence in a healthcare facility remains low if employees are overworked, undertrained, or lack support.
The issue is now about execution, not just information.
Following outbreaks, healthcare facilities must go beyond merely responding. Sustainable prevention needs:
• Consistent IPC training and skill evaluations
• Robust infection surveillance systems
• The availability of materials for safe injection
• Systems for monitoring and responsibility
• Campaigns to raise public awareness about the excessive use of injections
• Regulation of informal healthcare practitioners
If these steps are not taken, susceptible groups will continue to be at risk from avoidable healthcare-associated infections.
A Plea for Accountability in Moving Forward
The outbreaks in Taunsa and Ratodero serve as stark reminders that patient safety must be mandatory. Due to risky medical practices, children seeking treatment shouldn’t ever contract life-threatening infections.
Cooperation among healthcare practitioners, legislators, regulatory agencies, and communities is necessary to avoid future outbreaks. In particular, nurses have a significant role in fostering a culture of infection prevention at all levels of treatment.
Whether Pakistan is aware of the risks associated with unsafe injections is no longer the issue. The critical issue is whether healthcare systems are prepared to routinely implement safety procedures before another avoidable disaster happens.
References
In rural Pakistan, community involvement after a human immunodeficiency virus (HIV) epidemic: Challenges and lessons learned. Journal of the Pakistan Medical Association, 71(Suppl. 4), S31–S33. doi:10.47391/JPMA.0006. Altaf, A., Khursheed, A., Iftikhar, N., Farrukh, N., & Shah, S. A. (2021).
The BBC News. (2026, April 14). Undercover video revealed that the hospital at the epicenter of the child HIV epidemic was reusing syringes.
World Health Organization. (2019). Disease outbreak news: HIV outbreak in Larkana, Pakistan.
World Health Organization. (2022). Injection safety and the prevention of health care-associated infections.
Author Bio
Manghan Das is an Assistant Manager Infection Control at Shaheed Mohtarma Benazir Bhutto Institute of Trauma and is currently pursuing a Master of Science in Nursing (MSN) at Aga Khan University. He holds a Bachelor’s degree in Nursing and a Master’s degree in Hospital Administration. His professional interests include infection prevention and control, patient safety, hand hygiene, and healthcare quality improvement. He is passionate about nursing education and promoting evidence-based practices in healthcare settings.